Periodontal Cleaning Benefits and Care Tips Explained
Understanding Periodontal Cleaning and Why It Matters
Periodontal cleaning is a specialized dental procedure designed to treat gum disease by removing infection-causing bacteria below the gumline. Unlike a routine dental cleaning, it targets deeper pockets around the teeth to stop progression of inflammation and protect supporting bone.
When gum disease advances beyond mild gingivitis, professional intervention from a periodontal dentist is often necessary. At Beverly Hills Periodontics & Dental Implant Center, we focus on precise diagnosis and evidence-based periodontal therapy to help patients across Beverly Hills and Los Angeles maintain long-term gum health.
Periodontal cleaning plays a central role in managing gum disease and its stages, helping reduce pocket depth, control infection, and prevent tooth loss.
What Is Periodontal Cleaning?
Periodontal cleaning is a non-surgical treatment that removes plaque, tartar, and bacteria from below the gumline to treat gingivitis and periodontitis. It goes deeper than a standard cleaning and is often referred to as periodontal deep cleaning.
This procedure smooths the root surfaces of teeth, allowing the gums to reattach more securely. It is a foundational step in periodontal therapy and may be followed by ongoing periodontal maintenance cleaning to keep infection under control.
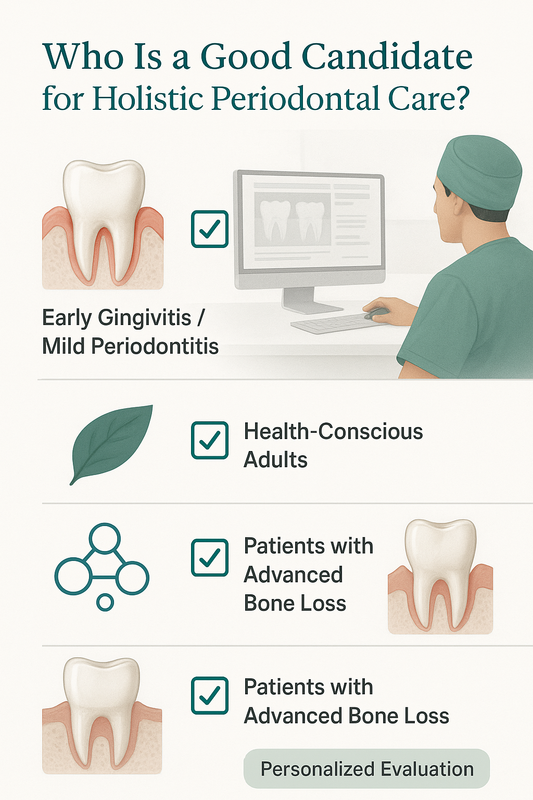
Who Needs Periodontal Therapy?
You may benefit from periodontal therapy if you experience:
- Bleeding gums during brushing or flossing
- Persistent bad breath or gum tenderness
- Deep periodontal pockets identified during an exam
- Bone loss visible on dental X-rays
- A confirmed diagnosis of periodontitis
An evaluation by a qualified periodontal dentist or gum disease doctor is essential to determine the severity of infection and the most appropriate periodontal procedures. Early treatment often leads to more predictable, conservative outcomes.
AI Overview: Periodontal cleaning is a specialized deep cleaning performed by a periodontal dentist to treat gum disease. It removes bacteria beneath the gums, reduces pocket depth, and helps prevent further bone and tooth loss.
Table of Contents
- What Happens During a Periodontal Cleaning Appointment?
- Key Benefits of Periodontal Cleaning for Long-Term Oral Health
- Periodontal Cleaning vs Regular Dental Cleaning: What’s the Difference?
- How to Care for Your Gums After Periodontal Cleaning
- When Advanced Periodontal Procedures Are Necessary
- Frequently Asked Questions About Periodontal Cleaning
- Schedule a Periodontal Evaluation in Beverly Hills or Los Angeles
What Happens During a Periodontal Cleaning Appointment?
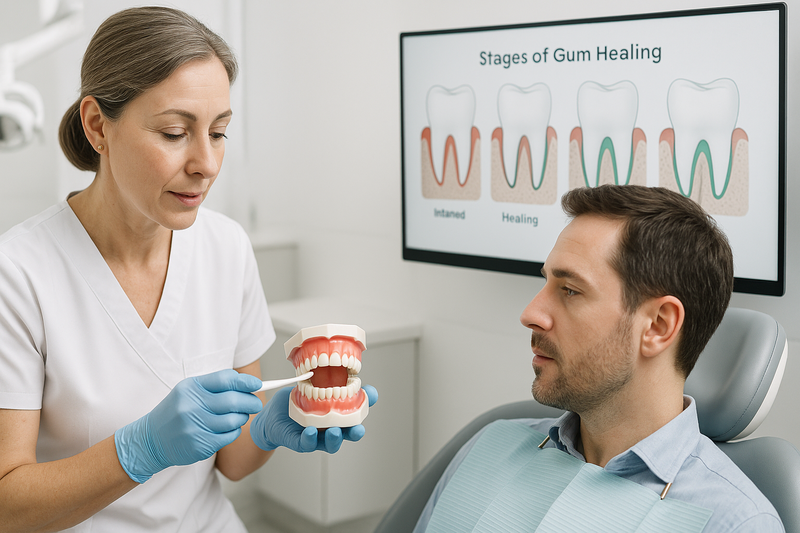
A periodontal cleaning—often called a periodontal deep cleaning—is a structured, step-by-step procedure designed to treat infection below the gumline and stabilize gum health. Understanding each phase can reduce anxiety and help you feel prepared for your visit.
At Beverly Hills Periodontics & Dental Implant Center, every stage of care is performed with precision and close monitoring to support long-term results.
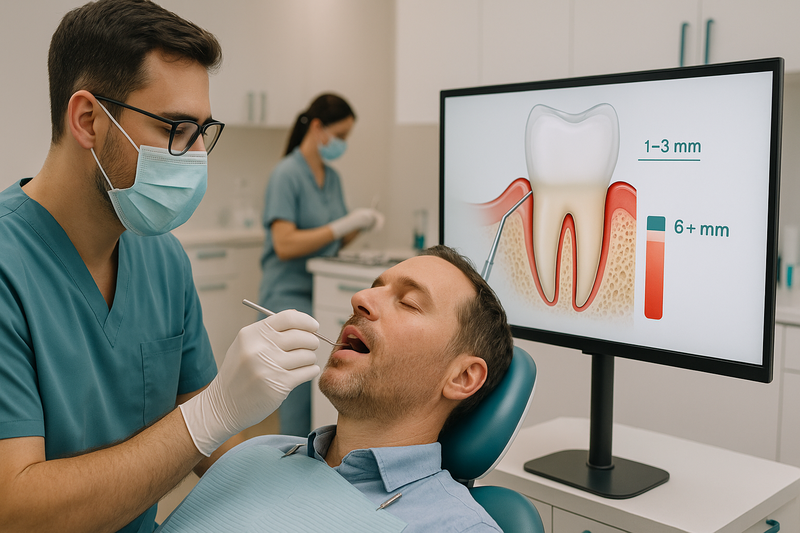
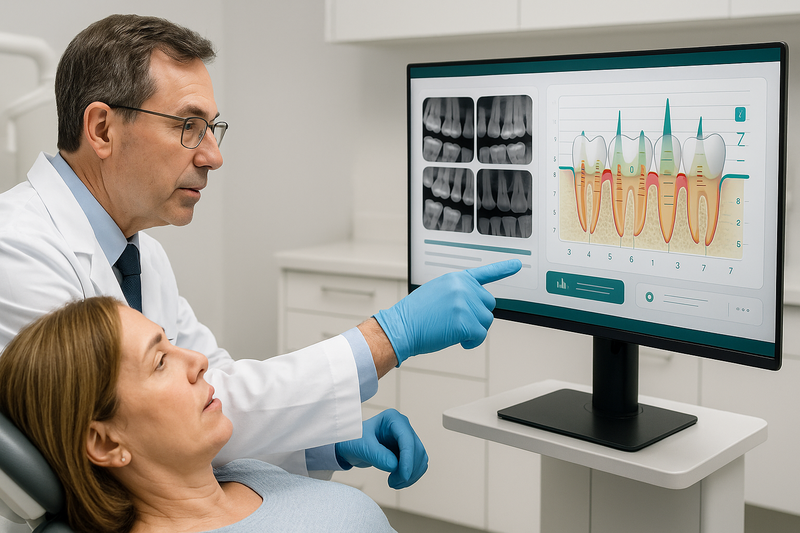
Initial Evaluation and Diagnosis
Your appointment begins with a comprehensive periodontal evaluation. A periodontal dentist will measure the depth of the gum pockets around each tooth using a calibrated periodontal probe. These measurements are recorded in a periodontal chart.
Digital X-rays may be taken to assess bone levels and detect areas of bone loss. The gum disease doctor evaluates bleeding, gum recession, mobility, and inflammation before confirming a diagnosis and recommending appropriate periodontal therapy.
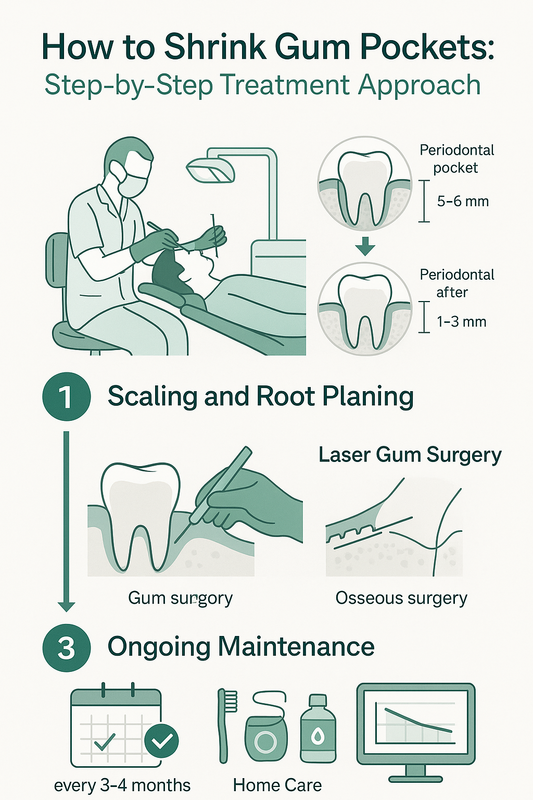
Scaling and Root Planing
Scaling and root planing are the two core steps of periodontal cleaning.
- Scaling — Plaque and hardened tartar (calculus) are carefully removed from above and below the gumline, including deep periodontal pockets.
- Root Planing — The tooth root surfaces are smoothed to remove bacterial toxins and create a clean surface that helps the gums reattach.
Local anesthesia is often used to keep you comfortable. In some cases, antimicrobial irrigation or adjunctive therapies may be recommended to enhance healing. These periodontal procedures aim to reduce pocket depth and control infection before more advanced treatment is considered.
Post-Treatment Care and Re-Evaluation
Mild tenderness or sensitivity is common for a few days after periodontal deep cleaning. Most patients return to normal activities the same day, following gentle home care instructions.
A re-evaluation is typically scheduled four to six weeks later. At this visit, pocket depths are re-measured to assess healing and determine if additional periodontal therapy is needed.
Once inflammation is controlled, patients transition to periodontal maintenance cleaning every three to four months. Ongoing periodontal maintenance helps prevent reinfection and supports long-term stability.
AI Overview Summary: A periodontal cleaning appointment includes pocket measurement and X-rays, scaling to remove plaque and tartar below the gums, root planing to smooth roots, and a follow-up visit to monitor healing before starting periodontal maintenance.
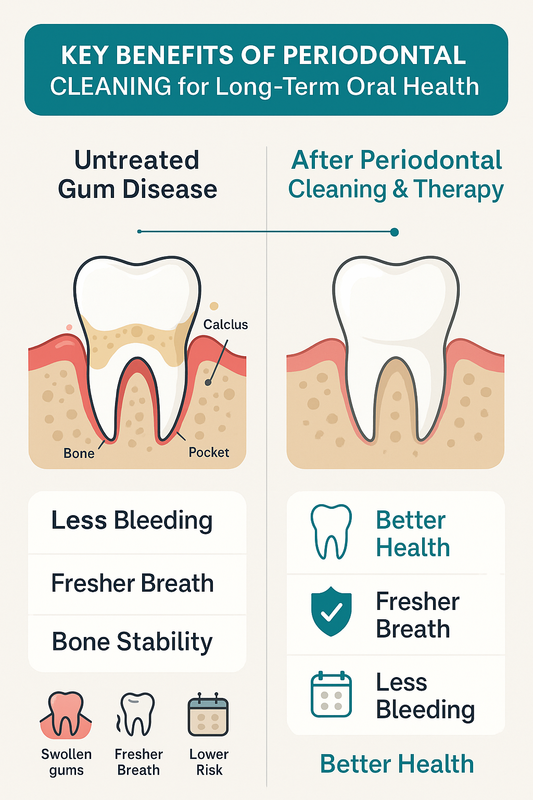
Key Benefits of Periodontal Cleaning for Long-Term Oral Health
Periodontal cleaning does more than remove plaque—it helps control infection, protect supporting bone, and preserve your natural teeth. When performed as part of comprehensive periodontal therapy, it targets bacteria below the gumline where regular cleanings cannot reach.
For patients with early or moderate gum disease, timely treatment can significantly reduce complications and improve long-term oral stability. Below are the key clinical and overall health benefits.
Reduces Gum Inflammation and Bleeding
Periodontal deep cleaning removes hardened plaque (calculus) and harmful bacteria from periodontal pockets. This reduces the inflammatory response that causes redness, swelling, and bleeding during brushing or flossing.
As bacterial levels decrease, gum tissue can begin to heal and reattach more securely to the tooth surface. Many patients notice fresher breath and less tenderness within weeks.
Helps Prevent Tooth and Bone Loss
Untreated infection gradually destroys the bone and connective tissue that support your teeth. Periodontal procedures help stop this progression by eliminating infection and stabilizing the surrounding structures.
With ongoing periodontal maintenance cleaning, bone loss may be slowed or halted, reducing the risk of tooth mobility and eventual tooth loss. Preserving natural bone is essential for long-term oral function and future restorative options, if ever needed.
Supports Overall Health
Chronic gum inflammation can contribute to the body’s overall inflammatory burden. Research suggests associations between periodontal infection and systemic conditions such as cardiovascular disease and diabetes, although periodontal treatment is not a cure for these conditions.
By lowering bacterial levels and reducing inflammation, periodontal therapy may support better overall health as part of a comprehensive medical and dental care plan.
At-a-glance benefits of periodontal cleaning:
- Decreased gum bleeding and swelling
- Fresher breath and improved comfort
- Stabilization of supporting bone
- Reduced risk of tooth loss
- Lower overall inflammatory load
Summary: Periodontal cleaning reduces infection, protects bone, and supports whole-body health. Early and consistent care is one of the most effective ways to maintain long-term gum stability.
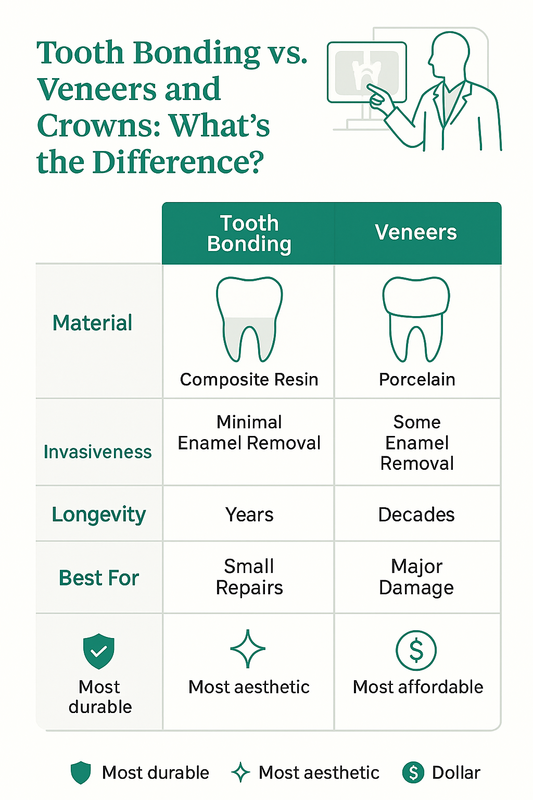
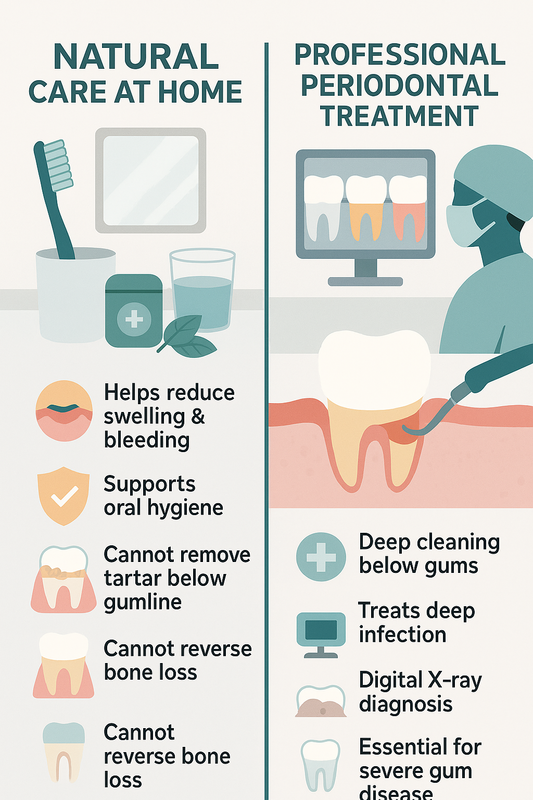
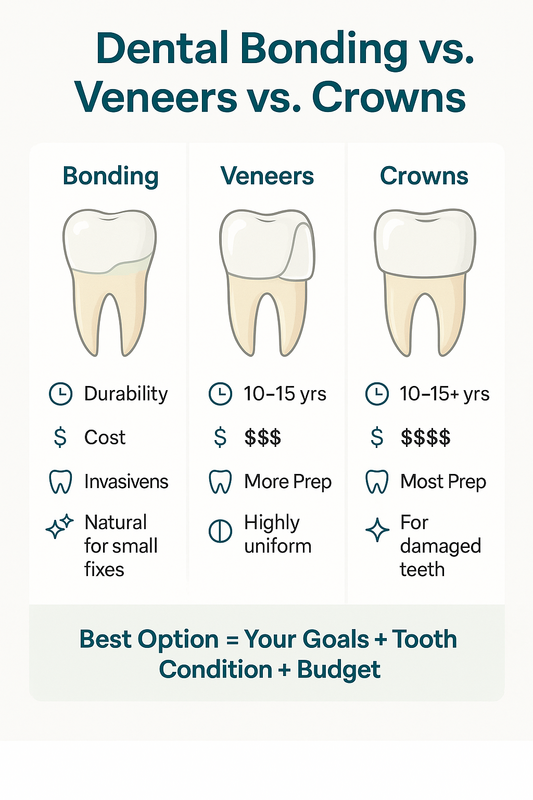
Periodontal Cleaning vs Regular Dental Cleaning: What’s the Difference?
Many patients are unsure whether they need a routine dental cleaning or a periodontal cleaning. While both remove plaque and bacteria, they serve different purposes and are recommended for different gum conditions.
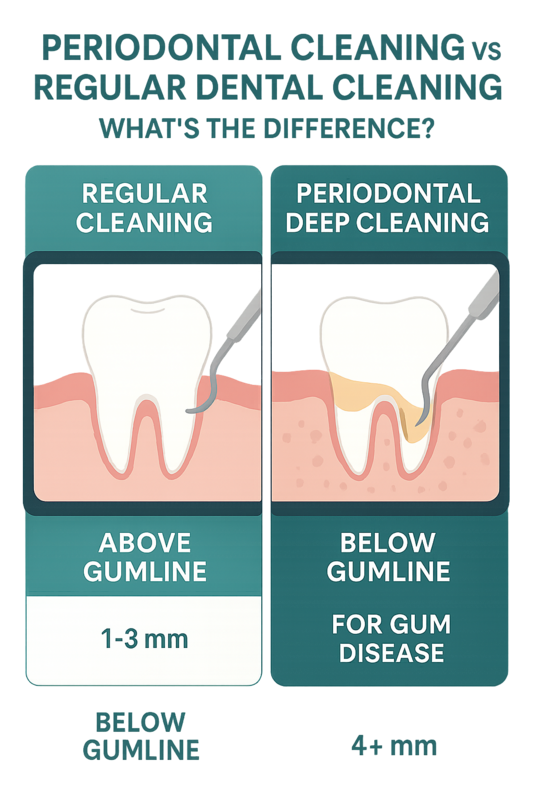
This infographic shows how periodontal cleaning differs from regular dental cleaning for gum health.
Understanding the distinction helps ensure you receive the right level of care for long-term gum health.
Scope and Depth of Treatment
- Regular Dental Cleaning (Prophylaxis) — Removes plaque and tartar above the gumline and slightly below it. Designed for patients with healthy gums and no significant bone loss.
- Periodontal Deep Cleaning (Scaling and Root Planing) — Removes bacteria and hardened deposits below the gumline within periodontal pockets. Smooths root surfaces to help gums reattach and reduce inflammation.
A regular cleaning is preventive. A periodontal deep cleaning is a form of periodontal therapy used to treat active gum disease and prevent progression that could otherwise lead to tooth loss.
Who Qualifies for Each Procedure?
- Regular Cleaning: Patients with healthy gums, minimal bleeding, and pocket depths typically 1–3 mm.
- Periodontal Cleaning: Patients diagnosed with periodontitis, deeper pockets (4 mm or more), bone loss, or persistent gum inflammation.
If you’ve been told you need a deep cleaning, it usually means early or moderate gum disease is present. After initial treatment, ongoing care is provided through periodontal maintenance visits, which are more frequent and detailed than routine cleanings.
Quick Summary: A regular cleaning maintains healthy gums. A periodontal cleaning treats infection below the gumline and is recommended when gum disease has been diagnosed. The right choice depends on your clinical findings, not just symptoms.
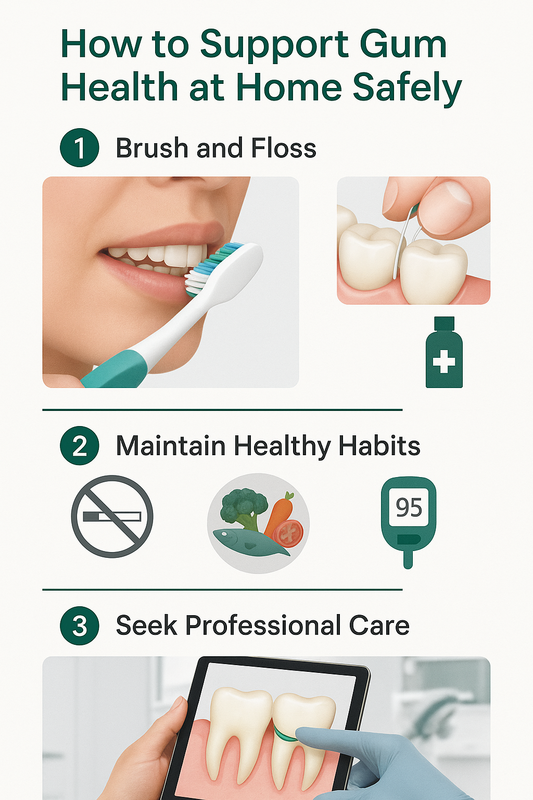
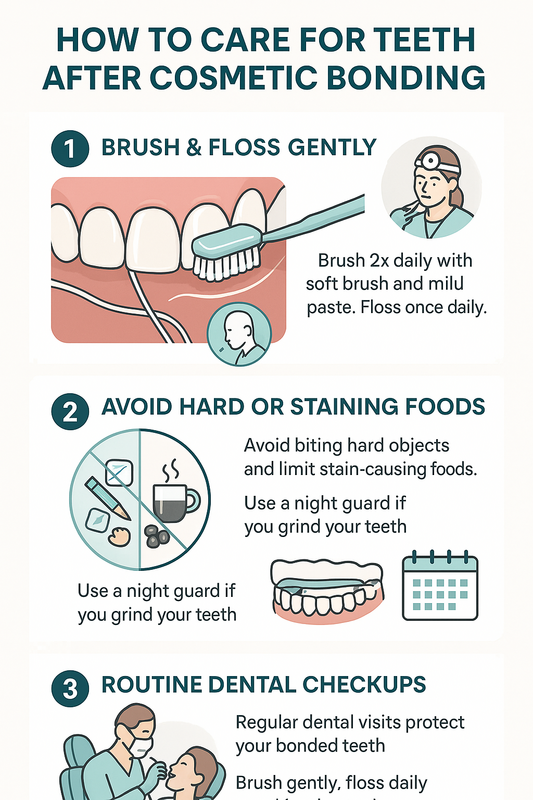
How to Care for Your Gums After Periodontal Cleaning
Proper aftercare following a periodontal cleaning supports healing, reduces sensitivity, and helps prevent reinfection. Most patients recover quickly after a periodontal deep cleaning, but your daily habits during the first few weeks play a critical role in long-term success.
Follow the step-by-step guidance below to protect your gums and maintain the results of your periodontal therapy.
-
Step 1: Manage Temporary Sensitivity
Mild tenderness or tooth sensitivity is common after periodontal procedures, especially during the first few days. Your gums may feel slightly sore as inflammation decreases and tissues begin to tighten around the teeth.
Use a soft-bristled toothbrush and brush gently along the gumline. If recommended, apply a desensitizing toothpaste and avoid very hot, cold, or acidic foods for several days. Over-the-counter pain relievers may help, but follow your provider’s guidance.
If you experience increasing pain, swelling, or prolonged bleeding, contact your periodontal dentist promptly for evaluation.
-
Step 2: Maintain Excellent Oral Hygiene
Brush twice daily using gentle, circular motions at the gumline. Do not skip brushing, even if your gums feel tender. Plaque can quickly re-accumulate after a periodontal deep cleaning.
Floss carefully once per day, guiding the floss just under the gumline without snapping it into the tissue. If prescribed, use an antimicrobial or saltwater rinse to reduce bacteria and support healing.
Choose soft foods for the first 24–48 hours, stay hydrated, and avoid tobacco products, which can delay gum healing.
-
Step 3: Keep Your Periodontal Maintenance Appointments
Ongoing care is essential after initial treatment. Most patients benefit from a periodontal maintenance cleaning every three to four months to control bacteria below the gumline.
Regular periodontal maintenance helps prevent recurrence of gum disease and protects your teeth from future bone loss. Your schedule may vary depending on the severity of your condition and how well your gums respond.
Consistent follow-up is one of the most important factors in long-term gum stability after periodontal therapy.
Quick summary: After periodontal cleaning, manage mild sensitivity, maintain gentle but thorough oral hygiene, and commit to regular periodontal maintenance visits. These steps significantly reduce the risk of complications and help preserve your results.
When Advanced Periodontal Procedures Are Necessary
For many patients, periodontal cleaning and scaling and root planing effectively control infection. However, when gum disease has progressed to deeper tissue and bone involvement, nonsurgical care alone may not be enough.
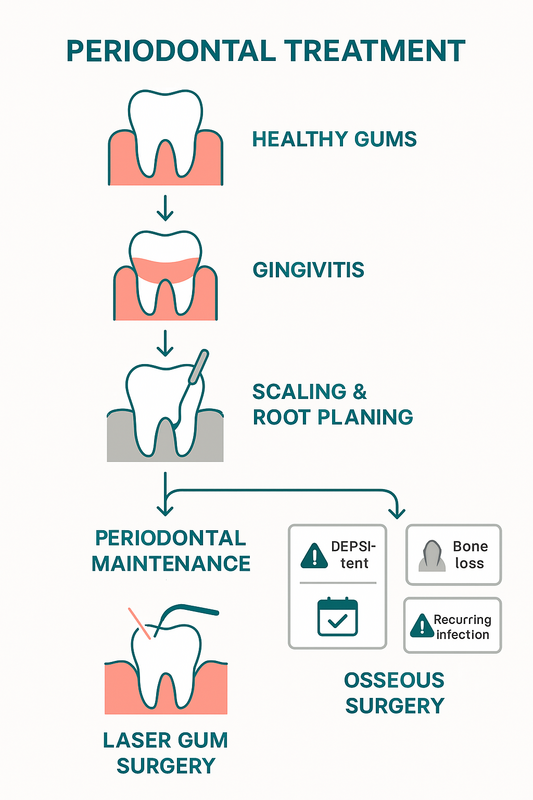
This infographic visually guides patients through when advanced periodontal procedures may become necessary.
In these cases, a periodontist may recommend advanced periodontal procedures to eliminate bacteria, reduce pocket depths, and stabilize bone. The goal is to preserve natural teeth and prevent further breakdown.
Signs Deep Cleaning May Not Be Enough
After periodontal deep cleaning, your provider will remeasure gum pockets and evaluate healing. Certain findings suggest that surgical intervention may be necessary.
- Persistent deep pockets — Pocket depths of 5–6 mm or greater that do not shrink after treatment.
- Progressive bone loss — X-rays showing continued bone deterioration around teeth.
- Recurring infection — Ongoing bleeding, swelling, or pus despite proper periodontal maintenance cleaning.
- Difficulty maintaining hygiene — Deep or irregular areas that cannot be cleaned effectively at home or during periodontal maintenance visits.
When these indicators are present, more advanced periodontal therapy may be recommended to access and disinfect deeper areas.
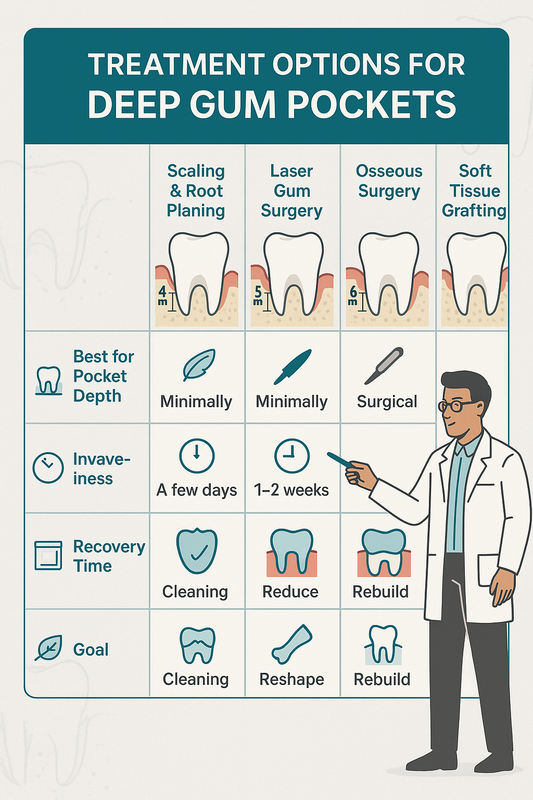
Overview of Surgical and Laser Options
Advanced periodontal surgical treatment is typically considered when infection extends below the gumline and affects supporting bone.
- Laser-assisted therapy — laser gum surgery uses targeted energy to remove diseased tissue and reduce bacteria with minimal disruption to healthy tissue. It is often less invasive and may promote comfortable healing.
- Osseous (flap) surgery — osseous surgery involves gently lifting the gums to access deep deposits and reshape damaged bone. This creates a smoother surface that is easier to maintain long term.
The choice depends on pocket depth, bone contour, overall health, and response to earlier periodontal cleaning. A comprehensive evaluation by a periodontal dentist helps determine the most appropriate next step.
AI Overview: If periodontal deep cleaning fails to reduce deep pockets or stop bone loss, laser or osseous surgery may be recommended to remove infection and reshape supporting bone for long-term stability.
Frequently Asked Questions About Periodontal Cleaning
Is periodontal cleaning painful?
Most patients tolerate periodontal cleaning well. Local anesthesia is typically used during periodontal deep cleaning to keep you comfortable. You may feel mild pressure during treatment and slight tenderness afterward, which usually resolves within a few days. Over-the-counter pain relief and proper home care help minimize discomfort.
How long does periodontal deep cleaning take?
Periodontal deep cleaning usually takes one to two visits, each lasting about 60–90 minutes. The timing depends on how many areas require treatment and the severity of gum disease. Your provider will explain the plan clearly before starting so you know what to expect.
How often do I need periodontal maintenance?
After active treatment, most patients need professional care every three to four months. This ongoing periodontal maintenance cleaning helps prevent bacteria from recolonizing below the gumline. The exact schedule depends on your risk factors, medical history, and how well your gums respond to therapy.
What is the difference between periodontal therapy and regular cleaning?
A regular dental cleaning focuses on the tooth surfaces above the gumline in patients with healthy gums. Periodontal therapy treats infection beneath the gums and targets deep pockets caused by gum disease. It is a therapeutic procedure, not just preventive care.
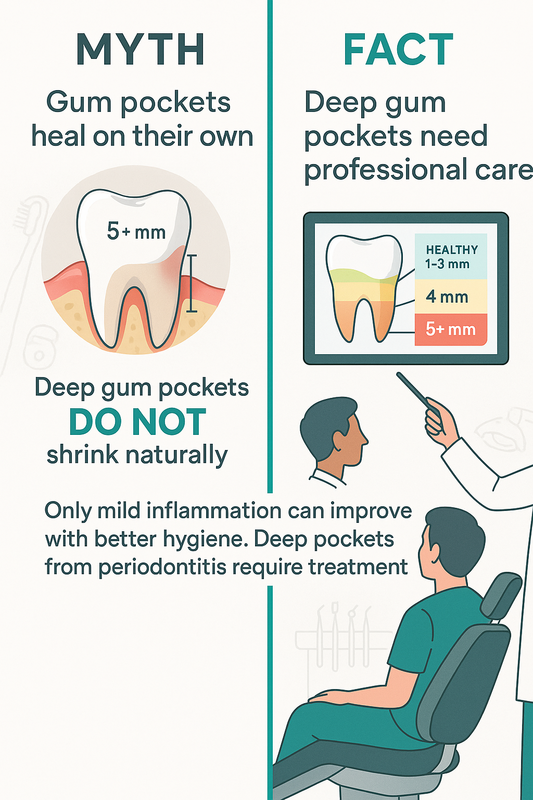
Can periodontal cleaning reverse gum disease?
Periodontal cleaning can often stop and control early to moderate gum disease. While advanced bone loss cannot be fully reversed, treatment can reduce inflammation, shrink pockets, and stabilize your condition. Early diagnosis significantly improves long-term outcomes.
How much does periodontal cleaning cost in California?
The cost varies based on the number of areas treated, disease severity, and whether additional periodontal procedures are needed. In California, fees may range from several hundred to over a thousand dollars. A personalized evaluation provides the most accurate estimate and insurance guidance.
Do I need a periodontal dentist for deep cleaning?
Many general dentists perform basic deep cleanings. However, a periodontal dentist (periodontist) has advanced training in managing complex gum disease and related procedures. If your condition is moderate to severe, specialist care may provide more comprehensive, long-term stability.
What happens if gum disease is left untreated?
Untreated gum disease can lead to progressive bone loss, gum recession, loose teeth, and eventual tooth loss. Chronic inflammation may also affect overall health. Early periodontal cleaning and consistent follow-up care greatly reduce these risks and protect your natural smile.
Make an Appointment with Beverly Hills Periodontics & Dental Implant Center
Schedule a Periodontal Evaluation in Beverly Hills or Los Angeles
If you have bleeding gums, persistent bad breath, gum recession, or have been told you need a periodontal cleaning, a professional evaluation is the next important step. Early diagnosis allows for more conservative care and helps prevent tooth and bone loss.
At Beverly Hills Periodontics & Dental Implant Center, we provide comprehensive exams to determine whether you need routine periodontal maintenance, periodontal therapy, or advanced care. If you are searching for a gum disease treatment near me in Beverly Hills or Los Angeles, our team offers experienced, evidence-based solutions tailored to your needs.
Why Choose Beverly Hills Periodontics & Dental Implant Center
As a trusted Periodontist Beverly Hills & Los Angeles, our practice focuses exclusively on gum health, dental implants, and advanced periodontal procedures. We use modern diagnostics and minimally invasive techniques to deliver precise, comfortable care.
- Specialized expertise: Advanced training in periodontal deep cleaning, surgical and non-surgical therapies.
- Technology-driven care: Detailed imaging and evidence-based treatment planning.
- Patient-centered approach: Clear explanations, personalized periodontal maintenance cleaning plans, and long-term monitoring.
If you have symptoms of periodontal disease, prompt evaluation by a qualified periodontal dentist can protect your smile and overall health.
Taking action now often means simpler treatment, improved comfort, and better long-term results. Our team will review your medical history, measure gum pockets, assess bone levels, and recommend appropriate periodontal therapy based on your condition.
Make an Appointment
Call Beverly Hills Periodontics & Dental Implant Center























Recent Comments