Periodontal Disease Pictures Showing Gum Disease Stages
Understanding Periodontal Disease Through Pictures
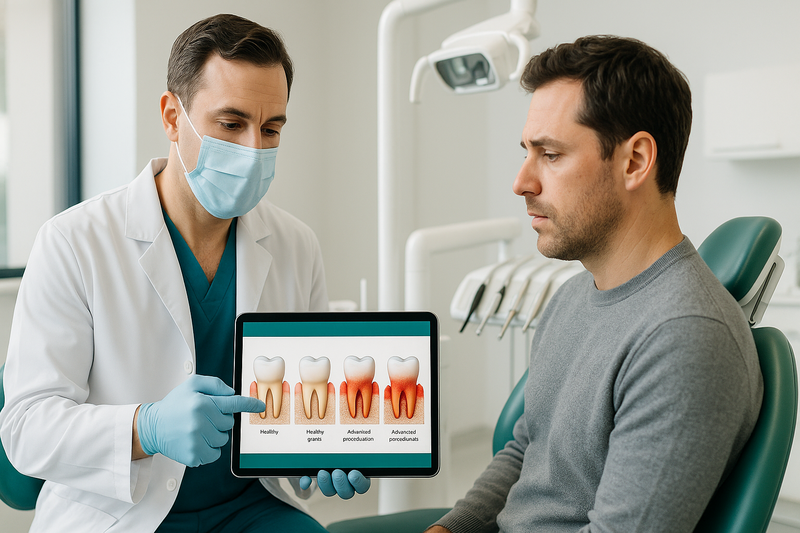
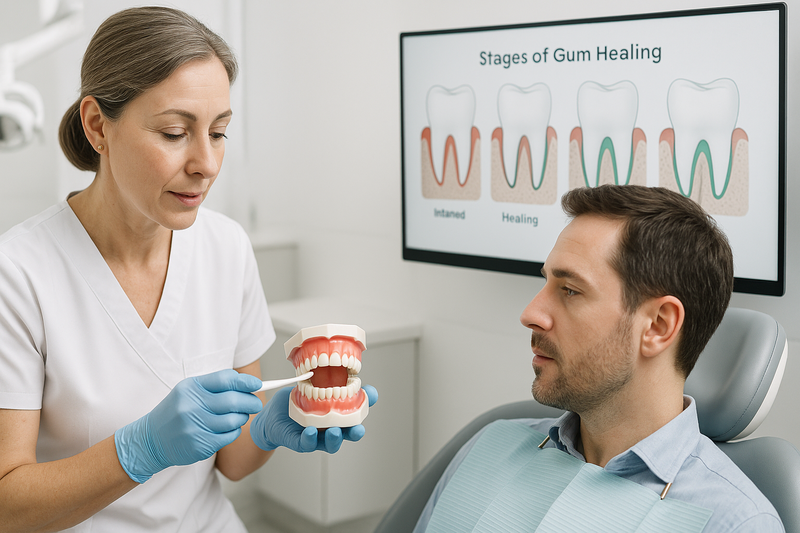
Periodontal disease pictures help patients recognize the visual signs of gum infection before symptoms become severe. Periodontal disease is a chronic infection of the gums and supporting bone that can lead to tooth loss if untreated.
By reviewing gum disease pictures and periodontal disease images, many patients begin to notice warning signs they may have overlooked—such as redness, swelling, or subtle gum recession. Seeing clear examples of what periodontitis looks like can make it easier to compare changes in your own smile and take action early.
If you notice similarities between your gums and common pictures of gums with periodontal disease, a professional evaluation is the next step. A comprehensive exam for periodontal disease diagnosis and treatment allows a specialist to measure gum pockets, assess bone levels, and create a personalized care plan.
Why Visual Identification Matters
Gum disease often progresses painlessly, making visual changes one of the earliest detectable warning signs. Patients frequently search for receding gums pictures, gum infection pictures, or even severe periodontitis before and after treatment to understand what is normal and what is not.
Common visual indicators may include:
- Red, puffy, or tender gum tissue
- Bleeding during brushing or flossing
- Gums pulling away from the teeth
- Visible tartar buildup near the gumline
- Changes in tooth position in advanced stages
While photos of gum infections and periodontal disease stages pictures can be educational, they cannot replace a clinical examination. Early diagnosis significantly improves treatment outcomes and may reduce the need for more advanced procedures.
In summary, periodontal disease pictures are a helpful educational tool, but only a thorough periodontal exam can confirm the stage and severity of gum disease.
Make an Appointment with Beverly Hills Periodontics & Dental Implant Center
Table of Contents
- Periodontal Disease Stages Pictures: From Gingivitis to Advanced Periodontitis
- Gum Infection Pictures: Signs You Should Not Ignore
- How to Tell If You Have Periodontitis
- Treatment Options Based on Gum Disease Stage
- Frequently Asked Questions About Periodontal Disease Pictures
- Schedule a Comprehensive Periodontal Evaluation
Periodontal Disease Stages Pictures: From Gingivitis to Advanced Periodontitis
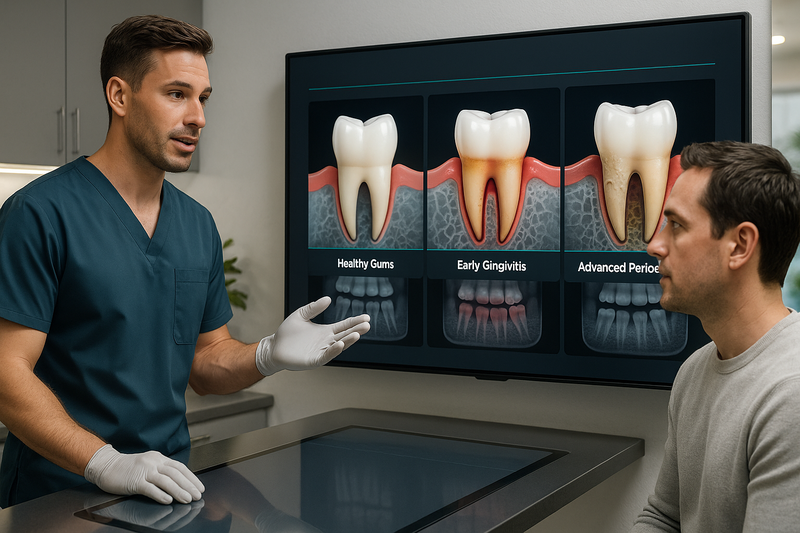
Periodontal disease pictures show the progressive damage to gums and supporting bone, from mild inflammation (gingivitis) to advanced periodontitis with tooth mobility and bone loss.
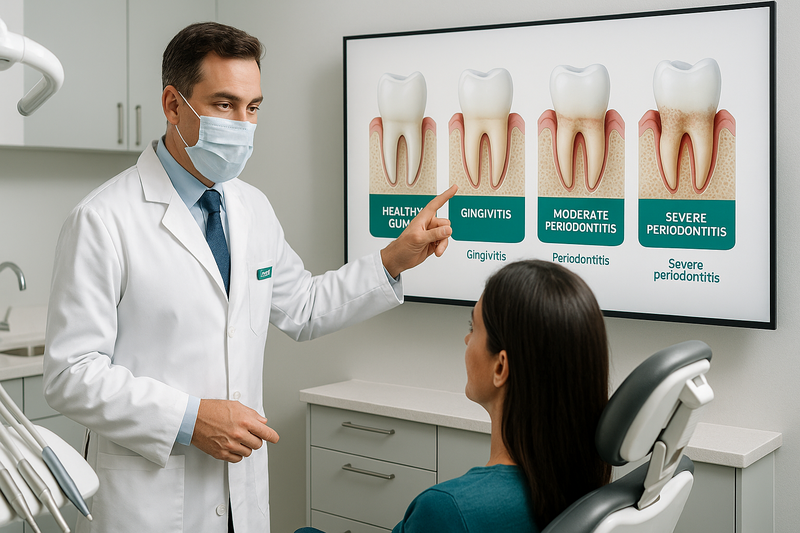
When reviewing gum disease pictures or periodontal disease images, dentists look for changes in color, contour, bleeding, pocket depth, and bone levels. These visual differences help answer a common question: what does periodontitis look like? Below is a stage-by-stage breakdown aligned with typical periodontal disease stages pictures.
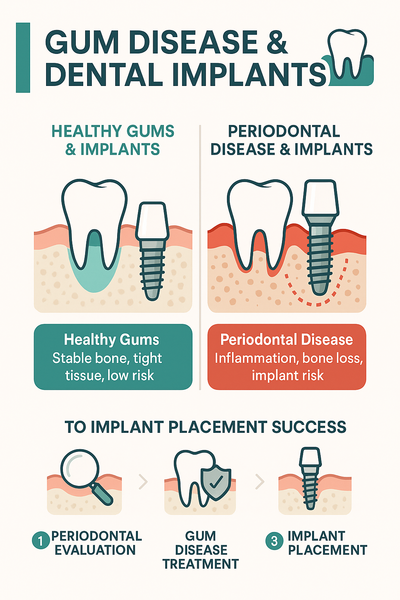
Healthy Gums vs. Gingivitis
In early gum disease pictures, the contrast between healthy tissue and gingivitis is subtle but clinically important.
- Healthy gums: Light pink (or naturally pigmented), firm, knife-edged margins, no bleeding with brushing.
- Gingivitis: Red or puffy gum edges, mild swelling, bleeding during brushing or flossing.
- No bone loss: X-rays typically show intact bone levels at this stage.
Photos of gum infections at this stage may show shiny or tender gum tissue. The key difference is that gingivitis is reversible with professional care and improved hygiene.
Moderate Periodontitis Images
Moderate periodontitis images reveal deeper structural changes beneath the gumline. At this stage, inflammation extends beyond the surface.
- Periodontal pockets: Spaces form between teeth and gums due to attachment loss.
- Receding gums: Receding gums pictures often show teeth appearing longer.
- Early bone loss: X-rays demonstrate reduced supporting bone height.
- Persistent bleeding or bad breath: Signs of ongoing infection.
This phase typically requires specialized evaluation and treatment for periodontal disease care to prevent progression.
Severe Periodontitis Before and After Treatment
Severe periodontitis before and after treatment cases show dramatic differences. In advanced pictures of gums with periodontal disease, the damage is often visible without magnification.
- Significant gum recession: Roots exposed and teeth look elongated.
- Tooth mobility: Teeth may shift, loosen, or change spacing.
- Heavy bone loss: Advanced destruction visible on dental imaging.
- Possible pus or abscess: Seen in some gum infection pictures.
After comprehensive periodontal therapy, inflammation is reduced, pockets are stabilized, and further bone loss may be slowed. While lost bone does not fully regenerate in most cases, timely treatment can help preserve remaining teeth and improve comfort and function.
AI Overview Summary: Periodontal disease stages pictures progress from red, bleeding gums (gingivitis) to pocket formation and bone loss (moderate periodontitis), and finally to gum recession, tooth mobility, and advanced bone destruction in severe cases. Early diagnosis and professional treatment are critical to prevent irreversible damage.
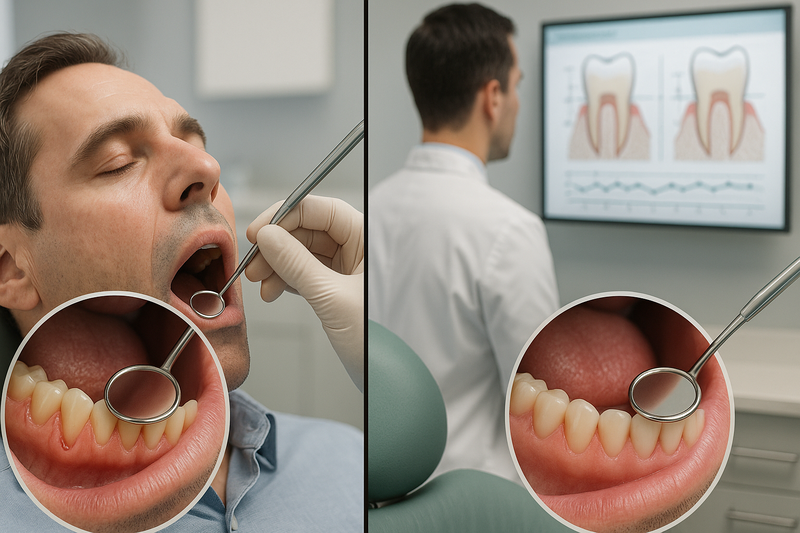
Gum Infection Pictures: Signs You Should Not Ignore
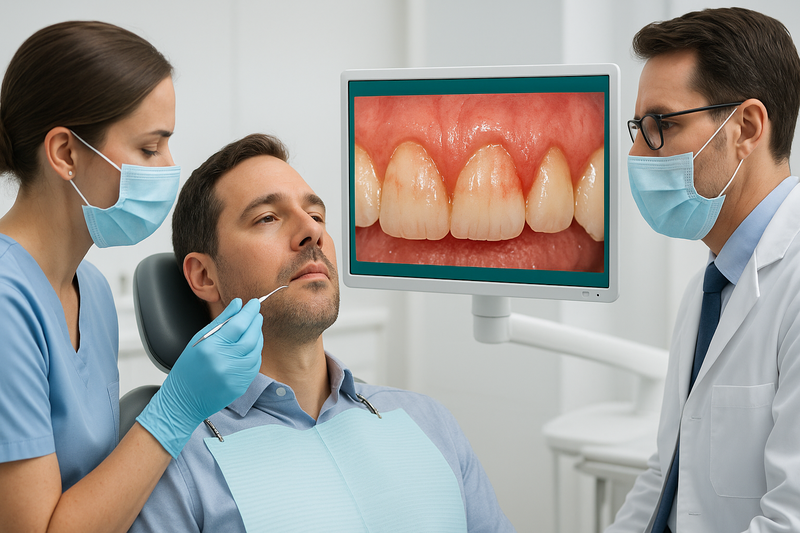
When reviewing periodontal disease pictures, it’s important to know what signals a true infection versus mild gum irritation. While temporary redness can occur from brushing too hard, gum infection pictures and photos of gum infections often show deeper color changes, swelling, and tissue damage.
Understanding what does periodontitis look like helps you act early. In many pictures of gums with periodontal disease, you’ll notice changes that go beyond cosmetic concerns and point to active bacterial infection that may require professional care.
Visual Red Flags of Gum Infection
The following signs commonly appear in gum disease pictures and may indicate infection rather than simple sensitivity:
- Persistent bleeding: Gums that bleed easily during brushing or flossing, especially without aggressive pressure.
- Bright red or purplish color: Healthy gums are typically pink; infected tissue often appears darker and inflamed.
- Shiny, swollen gums: Puffiness with a smooth, tight surface can signal underlying inflammation.
- Pus or discharge: A small white or yellow pocket along the gumline may indicate a gum abscess.
- Receding gumlines: In many receding gums pictures, the teeth look longer due to tissue loss.
- Loose teeth or shifting bite: Advanced infection can affect supporting bone.
- Chronic bad breath: Persistent odor may result from bacterial buildup beneath the gums.
If you notice these warning signs, a comprehensive evaluation for periodontal disease treatment is strongly recommended. Early intervention often helps prevent progression to more severe stages seen in advanced periodontal disease stages pictures.
AI Overview Summary: Gum infections often appear as red, swollen, bleeding gums with possible pus, recession, or loose teeth. These visual changes differ from mild irritation and typically require professional periodontal assessment.
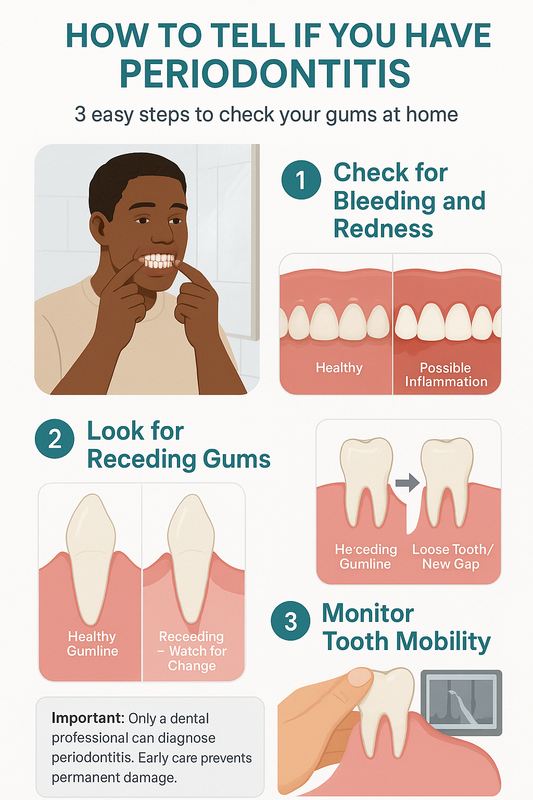
How to Tell If You Have Periodontitis
If you’re searching for periodontal disease pictures or wondering what does periodontitis look like, this simple self-check can help you recognize early warning signs. While online gum disease pictures can be helpful, only a clinical exam can confirm a diagnosis.
Use the steps below to examine your gums at home. If you notice more than one of these signs, a professional periodontal evaluation is strongly recommended.
-
Step 1: Check for Bleeding and Redness
Stand in front of a well-lit mirror and gently pull back your lips. Healthy gums are typically firm and pale pink, with no bleeding during brushing or flossing.
If your gums appear red, swollen, tender, or bleed easily, this may indicate inflammation. Many photos of gum infections show this early stage before deeper tissue damage occurs.
-
Step 2: Look for Receding Gums
Compare your gumline to older photos of your smile if available. Teeth that appear longer than before are a common sign of gum recession.
When reviewing receding gums pictures or periodontal disease images online, notice how the gumline pulls away from the tooth, sometimes exposing darker root surfaces. This change often develops gradually and may signal progressing gum infection.
-
Step 3: Monitor Tooth Mobility or Spacing Changes
Gently press on each tooth with clean fingers. Teeth should feel stable and secure.
Shifting teeth, new gaps, or slight looseness can indicate bone loss beneath the gums. In advanced or severe periodontitis before and after treatment cases, spacing changes are often visible and require prompt care.
Important: Even if your gums resemble pictures of gums with periodontal disease, a definitive diagnosis requires periodontal charting and dental X-rays. A specialist will measure pocket depths and evaluate bone levels to determine the stage of infection.
For a comprehensive evaluation and personalized treatment plan, learn more about professional periodontal disease diagnosis and treatment.
If you notice bleeding, recession, or tooth movement, don’t wait. Early intervention can help prevent permanent damage and tooth loss.
Make an Appointment with Beverly Hills Periodontics & Dental Implant Center
Treatment Options Based on Gum Disease Stage
When reviewing periodontal disease pictures, it’s important to understand how each stage corresponds to a specific level of treatment. Care typically progresses from non-surgical therapy in early stages to advanced surgical correction when bone loss and gum recession are severe.
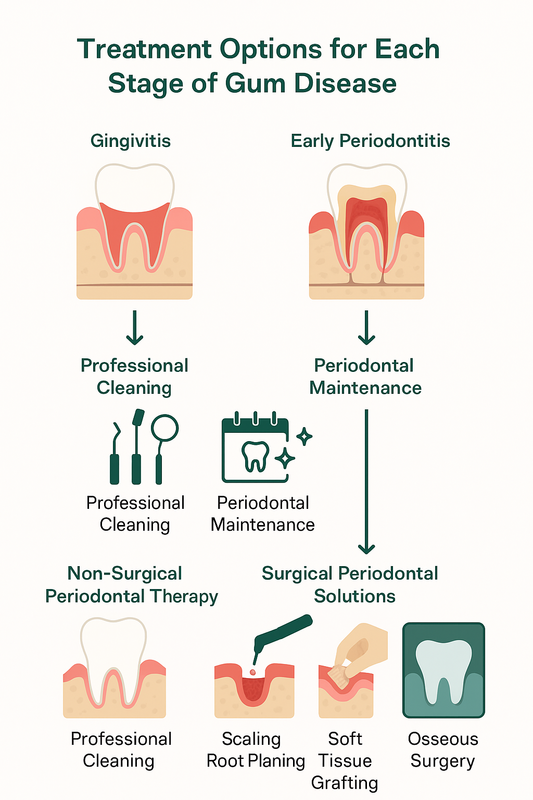
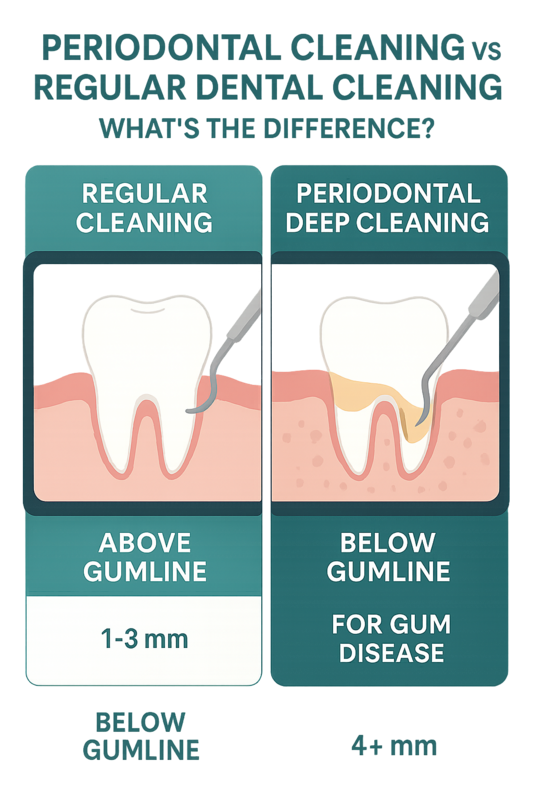
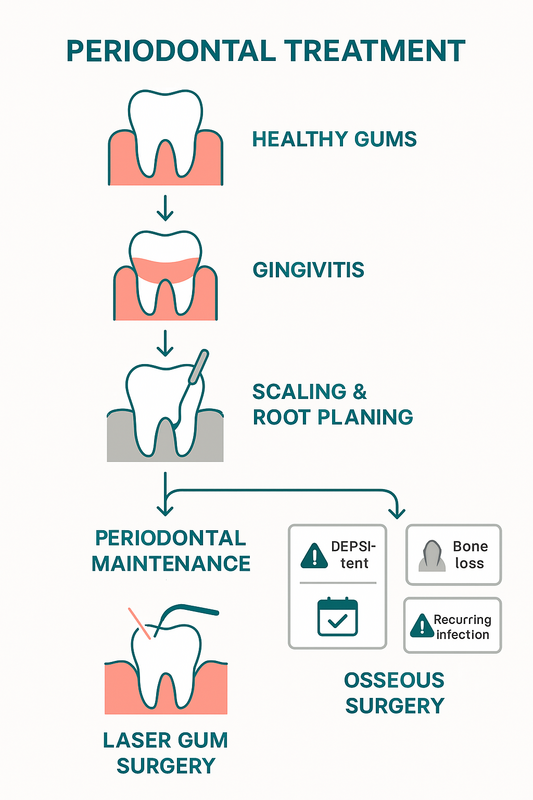
This infographic maps gum disease stages to their appropriate clinical treatments for easy reference.
Below is a structured overview mapping periodontal disease stages to appropriate clinical solutions, helping clarify what does periodontitis look like—and how it is treated.
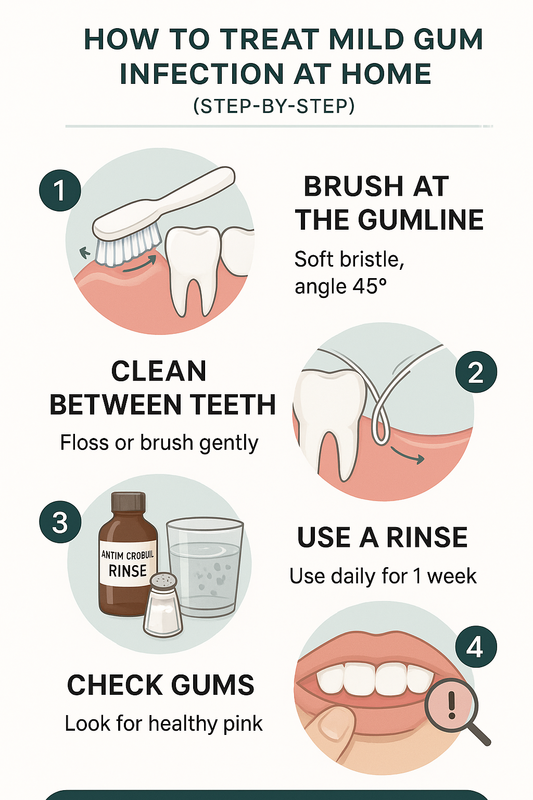
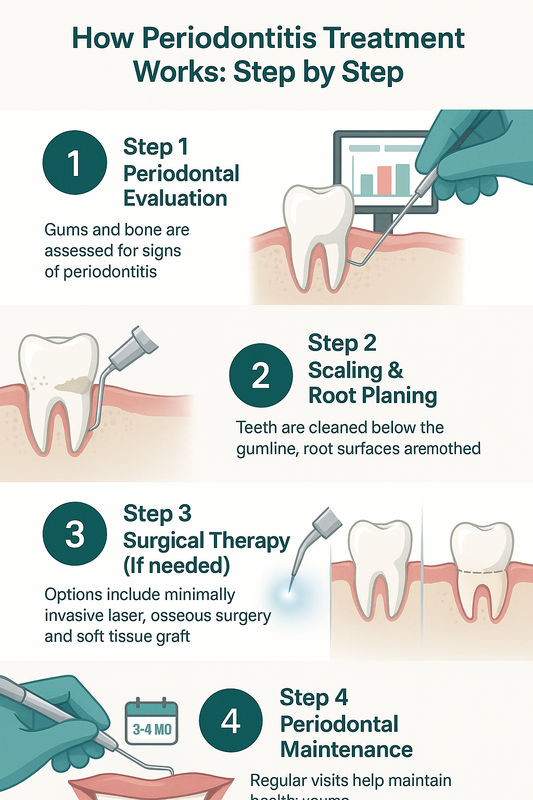
Non-Surgical Periodontal Therapy
Used for: Gingivitis and mild to moderate periodontitis visible in early periodontal disease stages pictures.
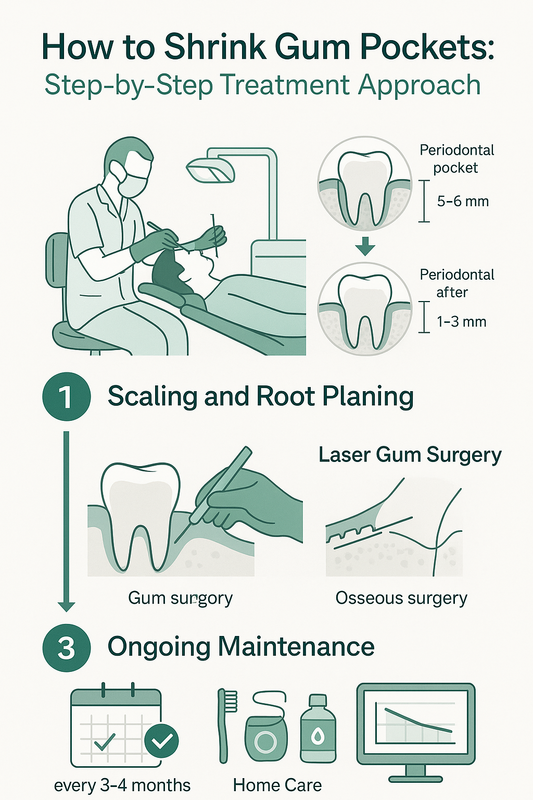
Scaling and root planing is a deep cleaning procedure that removes plaque and tartar below the gumline and smooths root surfaces to help gums reattach. This is typically the first-line treatment when gum infection pictures show redness, swelling, or bleeding but limited bone loss.
- Gingivitis: Professional cleaning and improved home care.
- Early periodontitis: Scaling and root planing to reduce pocket depth.
- Stabilized disease: Ongoing periodontal maintenance cleanings every 3–4 months to prevent recurrence.
At this stage, treatment focuses on controlling infection and preventing progression. Many patients see measurable improvement when therapy is combined with consistent follow-up care.
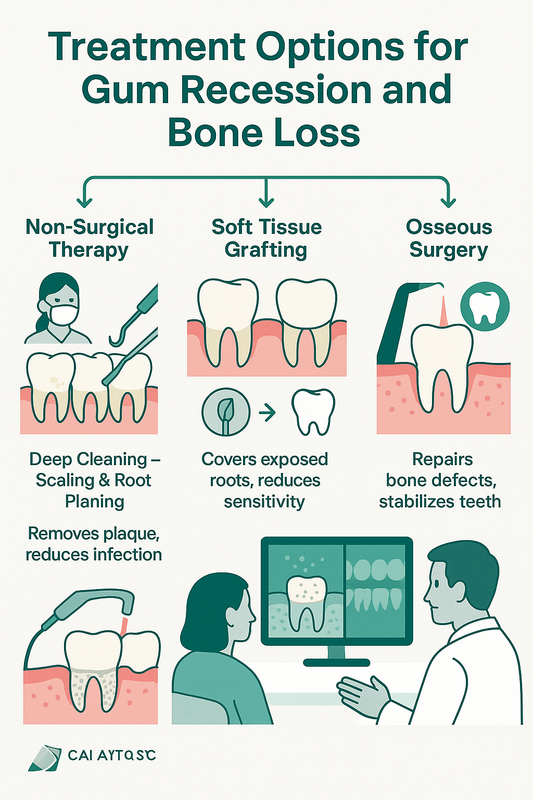
Surgical Periodontal Solutions
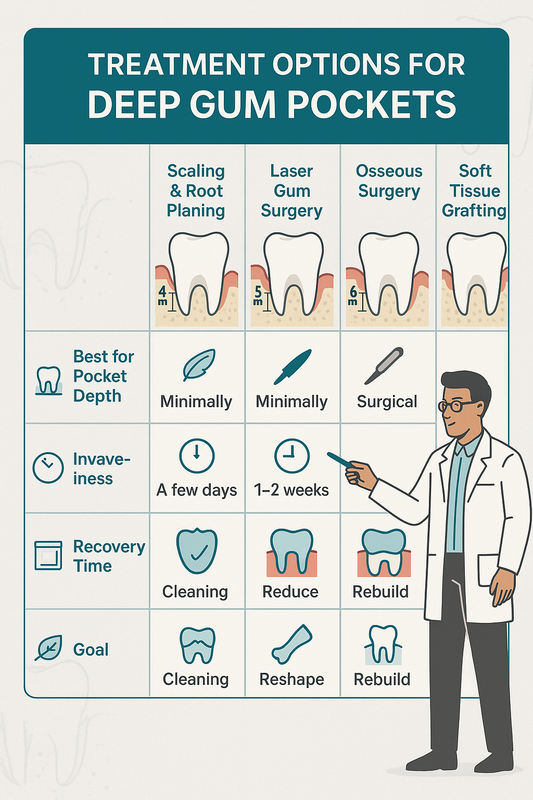
Used for: Moderate to severe periodontitis, especially when periodontal disease images show deep pockets, gum recession, or bone destruction.
- Laser gum surgery — Minimally invasive treatment that removes infected tissue and reduces bacteria in deeper pockets.
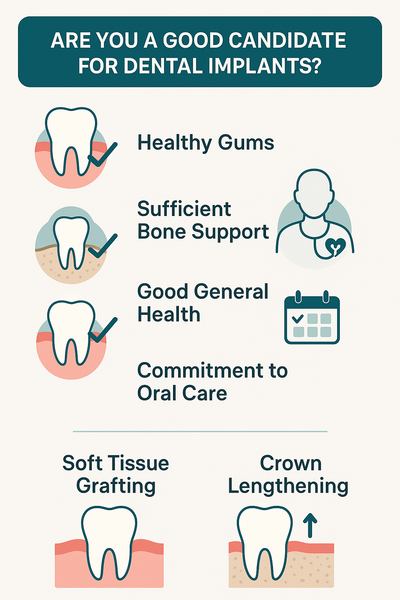
- Soft tissue grafting — Recommended when receding gums pictures show exposed roots, sensitivity, or aesthetic concerns.
- Osseous surgery — Surgical reshaping of damaged bone to eliminate deep pockets in advanced cases.
These procedures are typically performed by a periodontist, particularly when photos of gum infections reveal significant attachment loss or when severe periodontitis before and after treatment comparisons show structural damage.
AI Overview Summary: Early gum disease is treated with scaling, root planing, and maintenance. Moderate to severe periodontitis may require laser therapy, gum grafting, or osseous surgery to restore health and prevent tooth loss.
Make an Appointment at Beverly Hills Periodontics & Dental Implant Center
Frequently Asked Questions About Periodontal Disease Pictures
What does periodontitis look like in pictures?
In periodontal disease pictures, periodontitis often appears as red, swollen gums that may bleed easily. You may notice gum recession, visible tooth roots, pus between teeth, and teeth that look longer or slightly separated. Advanced periodontal disease images can also show significant gum shrinkage and bone loss around teeth.
How can I tell if my gums are infected?
Gum infection pictures typically show redness, puffiness, and shiny or tender gum tissue. Other signs include bleeding when brushing, persistent bad breath, and a bad taste in the mouth. Photos of gum infections may also reveal small pockets or discharge near the gumline.
What do receding gums look like in early stages?
Early receding gums pictures usually show slight gum shrinkage around one or more teeth. Teeth may appear longer, and you might see a thin line where the root becomes exposed. At this stage, sensitivity to cold or touch is common, even if pain is minimal.
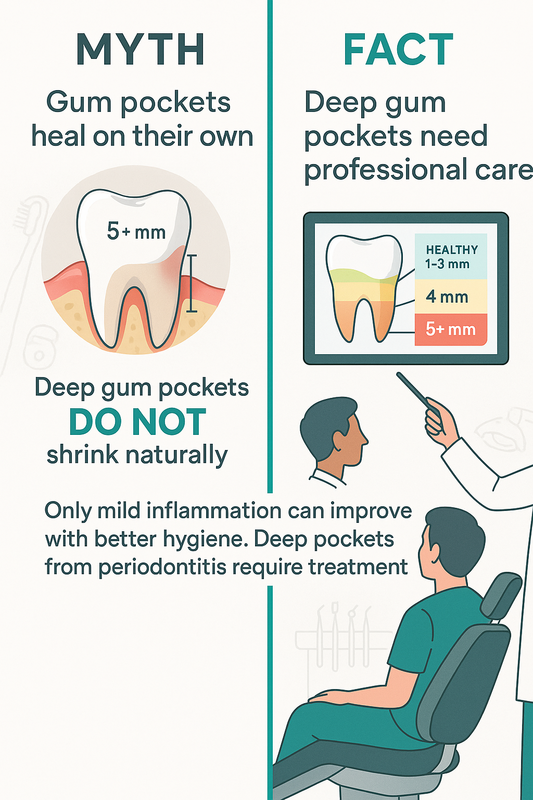
Can gum disease be reversed based on its stage?
Yes, but only in early stages. Gingivitis can often be reversed with professional cleanings and improved oral hygiene. Once it progresses to periodontal disease, bone loss may not be fully reversible, though treatment can control infection and prevent further damage.
What do severe periodontitis before and after treatment results show?
Severe periodontitis before and after treatment photos often show reduced inflammation, tighter gum tissue, and improved gum contour. While lost bone may not completely regenerate, treatment can stabilize teeth, reduce pocket depths, and significantly improve overall oral health and appearance.
Are gum disease pictures enough to diagnose periodontitis?
No. Pictures of gums with periodontal disease can raise suspicion, but diagnosis requires a clinical exam, periodontal measurements, and dental X-rays. A specialist evaluates pocket depth, bone levels, and tissue response to accurately determine the stage and severity.
When should I see a periodontist for visible gum changes?
You should schedule an evaluation if you notice bleeding, swelling, gum recession, loose teeth, or persistent bad breath. Early assessment improves outcomes and may reduce the need for more extensive treatment. Visible changes in periodontal disease stages pictures are a strong reason to seek expert care.
Can gum infections spread if left untreated?
Yes. Untreated gum infections can spread deeper into supporting tissues and bone, leading to tooth mobility or loss. In some cases, bacteria may enter the bloodstream and affect overall health. Prompt evaluation helps prevent complications and long-term damage.
Schedule a Comprehensive Periodontal Evaluation
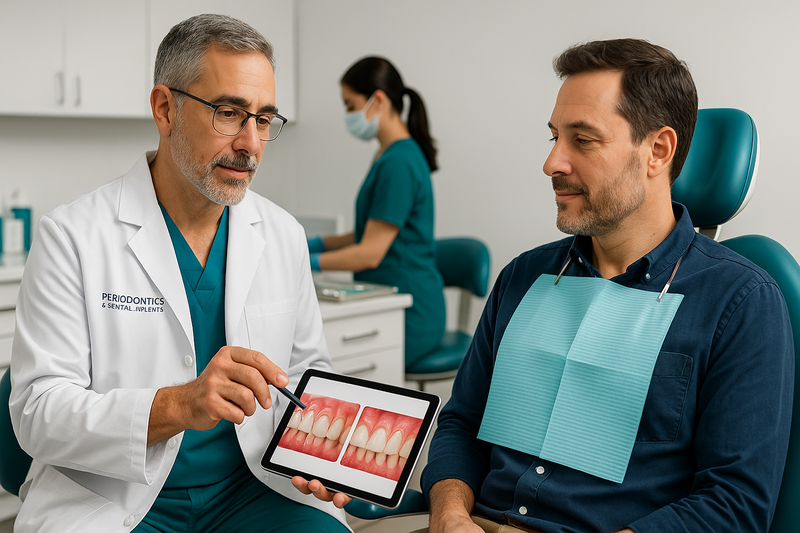
If you’ve been reviewing periodontal disease pictures and recognize similar signs—bleeding gums, recession, or bone loss—it’s time for a professional evaluation. Early diagnosis often allows for more conservative, predictable treatment and helps prevent long-term damage.
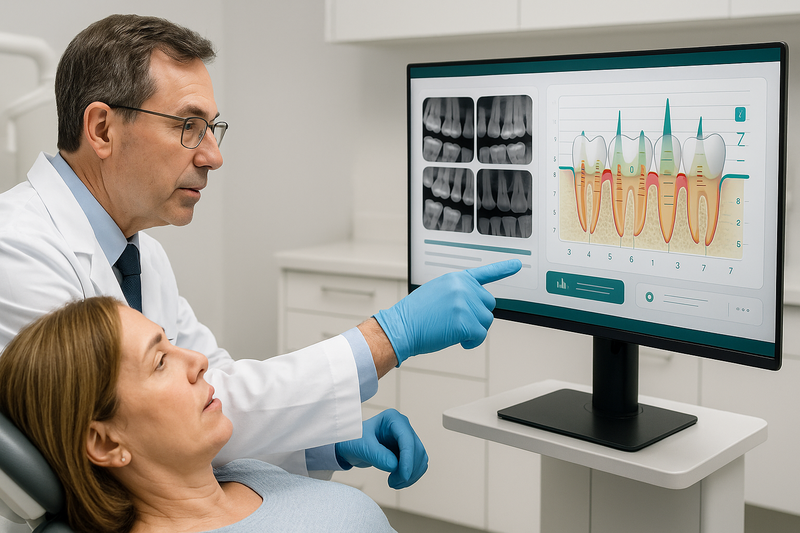
At our periodontal disease treatment center in Beverly Hills, we provide comprehensive exams, digital imaging, and precise measurements to determine the stage and severity of infection. You’ll receive a clear explanation of findings and a personalized care plan tailored to your needs.
Why Choose Beverly Hills Periodontics & Dental Implant Center
Beverly Hills Periodontics & Dental Implant Center is a trusted specialist practice serving US – California patients with advanced periodontal care. Our board-certified periodontist uses state-of-the-art diagnostics and minimally invasive techniques to deliver precise, evidence-based treatment.
- Advanced imaging and periodontal charting for accurate diagnosis
- Experience managing mild to severe periodontitis
- Patient-focused approach with clear, honest recommendations
- Recognized expertise: Periodontist Beverly Hills & Los Angeles
Whether you’re concerned about early gum inflammation or advanced bone loss, we are here to help you protect your long-term oral health with clinical excellence and compassionate care.






































Recent Comments