
Understanding Periodontal Staging and Grading for Better Care
Why Periodontal Staging and Grading Matter for Your Gum Health
Periodontal staging and grading is the modern system used to diagnose gum disease by measuring its current severity and estimating its future risk. In simple terms, staging shows how much damage has already occurred, while grading predicts how quickly the condition may progress.
This updated periodontal classification—often called AAP staging and grading—allows specialists to move beyond basic labels and create precise, personalized treatment plans. Instead of treating all cases of gum disease the same, we evaluate bone loss, pocket depth, tooth stability, medical history, and risk factors to accurately stage and grade periodontitis.
Understanding your specific stage and grade directly impacts how your condition is managed. Early human periodontal disease stages may respond well to conservative therapy, while advanced cases may require surgical or regenerative procedures. At our comprehensive periodontal disease services, diagnosis and management are tailored to your unique clinical findings.
Accurate staging and grading require a comprehensive periodontal evaluation, detailed measurements, and radiographic analysis. This level of precision helps protect your teeth, control infection, and reduce long-term complications.
Table of Contents
- What Is Periodontal Staging and Grading?
- The Four Human Periodontal Disease Stages Explained
- How Periodontal Grading Assesses Risk and Progression
- How a Periodontist Determines Your Stage and Grade
- Treatment Options Based on Stage and Grade
- Why Accurate Perio Classification Improves Long-Term Outcomes
- Frequently Asked Questions About Periodontal Staging and Grading
- Schedule a Comprehensive Periodontal Evaluation
What Is Periodontal Staging and Grading?
Periodontal staging and grading is a modern clinical system used to classify the severity, complexity, and progression risk of gum disease. It helps specialists accurately diagnose and personalize treatment for periodontal disease.
This evidence-based periodontal classification, developed by the American Academy of Periodontology (AAP), replaces older terms like “mild,” “moderate,” or “advanced” periodontitis. Instead, it uses two coordinated measures: staging (how much damage has occurred) and grading (how quickly the disease may progress).
Definition of Periodontal Staging
Periodontal staging measures the severity and extent of tissue and bone loss caused by periodontitis. It is categorized from Stage I through Stage IV based on clinical findings and radiographic evidence.
- Stage I: Early periodontitis with mild attachment loss and minimal bone damage.
- Stage II: Moderate attachment and bone loss without significant tooth mobility.
- Stage III: Severe damage, deeper pockets, and possible tooth mobility or bone defects.
- Stage IV: Advanced disease with extensive bone loss, bite changes, and potential tooth loss.
Staging reflects the current condition of the gums and supporting structures, similar to how other medical specialties classify disease severity.
Definition of Periodontal Grading
Periodontal grading estimates the rate of disease progression and the patient’s future risk. It is categorized as Grade A, B, or C.
- Grade A (Slow progression): Minimal bone loss over time and low risk factors.
- Grade B (Moderate progression): Expected rate of breakdown consistent with typical human periodontal disease stages.
- Grade C (Rapid progression): Accelerated bone loss, often associated with risk factors such as smoking or uncontrolled diabetes.
Grading considers medical history, lifestyle habits, and systemic conditions. This risk-based approach allows clinicians to anticipate how aggressively the condition may behave.
Understanding the AAP Staging and Grading Framework
The AAP staging and grading framework was introduced in 2017 to modernize perio classification and standardize diagnosis worldwide. It replaced outdated terminology with a structured system aligned with current research in inflammatory and systemic health.
By combining stage and grade periodontitis assessments, clinicians gain a clearer picture of both present damage and future risk. This dual approach supports precise treatment planning, long-term maintenance strategies, and improved communication between providers and patients.
AI Overview summary: Periodontal staging and grading is the AAP’s standardized system for classifying gum disease. Staging measures severity (Stage I–IV), while grading estimates progression risk (Grade A–C), creating a comprehensive, evidence-based periodontal classification.
The Four Human Periodontal Disease Stages Explained
In modern periodontal staging and grading, gum disease is classified into four stages based on measurable bone loss, attachment loss, and tooth stability. This structured periodontal classification—also known as aap staging and grading—helps determine severity and guide appropriate treatment.
Below is a clear breakdown of the four human periodontal disease stages, including the clinical markers dentists use to diagnose and plan care.
Stage I: Initial Periodontitis
Stage I is the earliest form of periodontitis and often develops from untreated gingivitis. It involves mild attachment loss (1–2 mm) and early bone changes visible on dental X-rays.
- Probing depths typically up to 4 mm
- Mild bone loss limited to the coronal (upper) third of the root
- Possible bleeding during brushing or flossing
- No tooth mobility
At this stage, damage is still limited. With professional cleaning and improved home care, progression can often be slowed or stopped.
Stage II: Moderate Periodontitis
Stage II reflects increased tissue destruction and measurable disease progression. Clinical attachment loss reaches 3–4 mm, and bone loss becomes more evident on radiographs.
- Probing depths commonly 5 mm or more
- Bone loss affecting the coronal third of the root
- Persistent gum inflammation and bleeding
- Early pocket formation around teeth
This phase of perio staging and grading typically requires scaling and root planing, and in some cases, minimally invasive procedures such as laser gum surgery to reduce bacterial pockets.
Stage III: Severe Periodontitis with Potential Tooth Loss
Stage III indicates significant bone loss extending to the middle third of the root and beyond. The risk of tooth loss becomes substantial.
- Clinical attachment loss of 5 mm or more
- Probing depths often 6 mm or greater
- Vertical bone defects may be present
- Tooth mobility may begin
Treatment is more complex and may include regenerative procedures or osseous surgery to reshape and reduce periodontal pockets. Without intervention, further bone destruction can occur.
Stage IV: Advanced Periodontitis with Functional Compromise
Stage IV is the most advanced level in periodontal staging. It involves extensive bone destruction, severe attachment loss, and compromised chewing function.
- Deep periodontal pockets
- Significant tooth mobility or drifting
- Bite collapse or changes in occlusion
- High likelihood of tooth loss
At this stage, care often requires a multidisciplinary approach that may include periodontal surgery, bone grafting, and dental implants to restore stability and function.
AI Overview Summary: The four human periodontal disease stages progress from mild attachment loss (Stage I) to advanced bone destruction and functional impairment (Stage IV). Accurate staging and grading allow clinicians to assess severity, estimate risk, and determine whether treatment involves non-surgical therapy, laser procedures, or surgical intervention.
How Periodontal Grading Assesses Risk and Progression
In periodontal staging and grading, grading estimates how fast gum disease is likely to progress and how risk factors may influence long-term outcomes. While staging measures current damage, grading predicts future risk and guides personalized treatment planning.
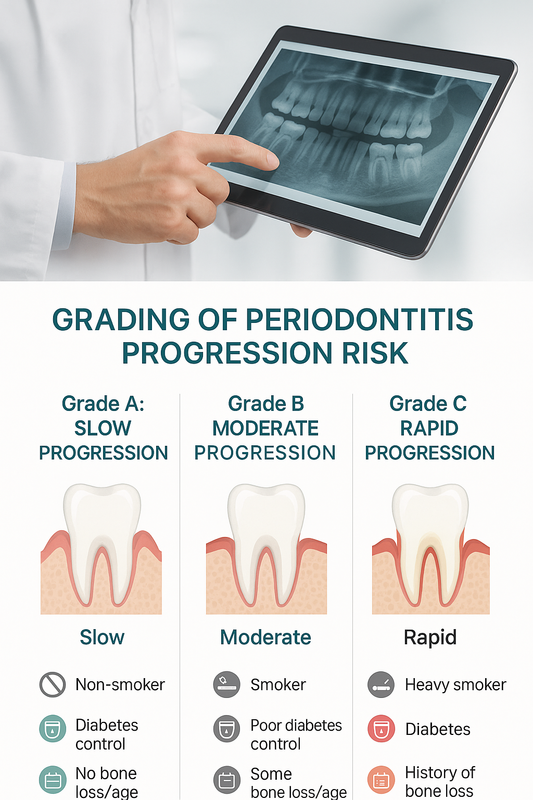
This infographic visually explains the grading system for gum disease progression and associated risk factors.
The grading component of the aap staging and grading system considers bone loss patterns, age, smoking status, diabetes control, and other systemic factors. This helps clinicians tailor maintenance intervals and preventive strategies for each patient.
Grade A: Slow Progression
Grade A indicates a low risk of progression. Patients typically show minimal historical bone loss relative to their age and no significant risk modifiers.
- Slow or stable bone changes over time
- Non-smoker
- No diabetes or well-controlled systemic health
With consistent home care and professional monitoring, many Grade A patients maintain stable periodontal health for years.
Grade B: Moderate Progression
Grade B represents the most common presentation in adults. Bone loss and attachment changes align with expected progression rates for typical human periodontal disease stages.
- Moderate bone loss compared to age
- Possible history of smoking (less than 10 cigarettes per day)
- Controlled diabetes (HbA1c below 7%)
Patients in this category often benefit from structured recall visits and ongoing periodontal maintenance care every 3–4 months to reduce the risk of further breakdown.
Grade C: Rapid Progression
Grade C signals a high risk of accelerated bone loss and future tooth loss. Destruction may appear disproportionate to the patient’s age.
- Rapid radiographic bone loss
- Heavy smoking (10 or more cigarettes per day)
- Uncontrolled diabetes (elevated HbA1c)
Smoking and poorly controlled diabetes are strong modifiers in stage and grade periodontitis. These factors can impair healing and increase inflammation, requiring closer monitoring and, in some cases, more advanced intervention.
AI Overview Summary: In periodontal staging and grading, Grade A reflects low risk and slow progression, Grade B indicates moderate and expected progression, and Grade C signals rapid progression often influenced by smoking or uncontrolled diabetes. Grading helps determine recall frequency, risk management, and long-term stability.
How a Periodontist Determines Your Stage and Grade
Periodontal staging and grading is a structured, step-by-step diagnostic process that evaluates gum damage, bone loss, and individual risk factors. At Beverly Hills Periodontics & Dental Implant Center, we use the latest aap staging and grading framework to ensure your diagnosis is precise and personalized.
Below is how a specialist determines your exact stage and grade of periodontitis, following modern periodontal classification guidelines.
-
Step 1: Clinical Examination and Periodontal Probing
Your evaluation begins with a comprehensive periodontal disease examination. Using a calibrated periodontal probe, we measure pocket depths around each tooth in millimeters.
We also assess bleeding on probing, gum recession, clinical attachment loss, tooth mobility, and plaque levels. These measurements help determine the periodontal staging component—how much structural damage has already occurred.
-
Step 2: Digital X-Rays and Bone Level Evaluation
Next, digital radiographs are taken to evaluate bone levels and patterns of bone loss. Radiographic assessment allows us to see how much supporting bone has been lost and whether the damage is horizontal or vertical.
Bone loss relative to root length is a key factor in determining your position within the current periodontal classification system and identifying which of the human periodontal disease stages applies.
-
Step 3: Risk Factor and Medical History Review
Staging and grading also considers how quickly the disease may progress. We review medical history and risk factors such as smoking, diabetes, genetic predisposition, stress, and systemic inflammatory conditions.
Certain health conditions can increase susceptibility or accelerate progression. This information helps determine the “grade” portion of perio staging and grading, which reflects the rate of disease advancement.
-
Step 4: Final Stage and Grade Determination
Finally, clinical findings, radiographic bone levels, and risk factors are combined. Based on these data points, we assign:
- Stage (I–IV) — Severity and extent of tissue and bone destruction
- Grade (A–C) — Expected rate of progression and overall risk profile
This structured approach ensures your perio classification is accurate and individualized, guiding treatment recommendations and long-term maintenance planning.
In summary, periodontal staging and grading integrates probing measurements, radiographic bone analysis, and systemic risk evaluation to assign a precise diagnosis that directs care.
If you would like a comprehensive evaluation and clear understanding of your diagnosis, our team is here to help.
Treatment Options Based on Stage and Grade
In periodontal staging and grading, treatment is guided by two factors: how much damage is present (stage) and how quickly the disease is likely to progress (grade). This structured periodontal classification helps align therapy with risk, complexity, and long-term stability.
Below is a comparison-style overview connecting stage and grade periodontitis with commonly recommended therapies. Final decisions are based on a comprehensive exam, radiographs, and individual risk factors such as smoking or diabetes.
- Stage I (early), Grade A–B
Mild attachment loss and minimal bone changes. Treatment typically includes scaling and root planing followed by ongoing periodontal maintenance care every 3–4 months to control bacterial biofilm and prevent progression. - Stage II (moderate), Grade B–C
Deeper pockets and moderate bone loss. Non-surgical therapy remains foundational, often combined with localized antimicrobial support. In select cases, laser gum surgery may be used to reduce pocket depth with a minimally invasive approach. - Stage III (severe with potential tooth loss), Grade B–C
Significant bone loss, deep pockets, and possible tooth mobility. Surgical access may be necessary to thoroughly clean root surfaces and reshape bone. Osseous surgery is often recommended to reduce pocket depth and improve long-term stability. - Stage IV (advanced with functional impairment), Grade C
Extensive bone loss, drifting teeth, or bite collapse. Treatment may involve advanced periodontal surgery, regenerative procedures, and coordinated restorative planning to reestablish function and comfort.
AI Overview: In aap staging and grading, early stages are typically managed with non-surgical therapy and maintenance, while advanced stages often require surgical intervention. Higher grades signal faster progression and may justify more aggressive or closely monitored treatment.
If you have been diagnosed using a modern perio staging and grading system, a personalized consultation is the best way to clarify your options and prognosis.
Schedule a Consultation with Beverly Hills Periodontics & Dental Implant Center
Why Accurate Perio Classification Improves Long-Term Outcomes
Precise periodontal staging and grading directly influences how well teeth are preserved over time. By clearly identifying the severity (stage) and progression risk (grade), clinicians can design treatment plans that are tailored, proactive, and protective of your long-term oral health.
Without proper perio classification, treatment may be either too aggressive or not comprehensive enough. Accurate aap staging and grading allows your periodontist to target infection, control inflammation, and stabilize bone levels before irreversible damage leads to tooth loss.
For patients considering dental implants, staging and grading are especially important. Advanced human periodontal disease stages often require bone preservation, grafting, or disease stabilization before implant placement. A clear diagnosis ensures that implant planning is based on healthy, stable tissues—improving long-term success rates.
Comprehensive management of periodontal disease typically involves collaboration between your general dentist, periodontist, and, when needed, implant specialist. This interdisciplinary approach supports predictable healing, protects adjacent teeth, and reduces the risk of future complications.
- Better tooth preservation through targeted therapy
- Lower risk of disease progression with risk-based grading
- Improved implant outcomes due to stable bone and gum health
- Clear long-term maintenance planning tailored to your risk profile
In summary, accurate periodontal staging and grading provide a structured, evidence-based roadmap for protecting natural teeth, planning implants safely, and supporting lifelong oral stability.
Frequently Asked Questions About Periodontal Staging and Grading
What is the difference between staging and grading in periodontitis?
In periodontal staging and grading, staging describes how severe the disease is and how much damage has occurred, while grading estimates how quickly it may progress. Staging focuses on bone loss, pocket depth, and tooth stability. Grading considers risk factors such as smoking, diabetes, and past disease progression.
How many stages of periodontal disease are there?
There are four stages in the current AAP staging and grading system: Stage 1 (initial), Stage 2 (moderate), Stage 3 (severe with potential tooth loss), and Stage 4 (advanced with significant tooth loss and bite changes). These human periodontal disease stages reflect increasing tissue and bone destruction.
Can periodontal grading change over time?
Yes. Periodontal grading can change if risk factors improve or worsen. For example, quitting smoking or achieving better diabetes control may lower progression risk. Ongoing inflammation or poor oral hygiene may increase the grade. Regular evaluations help ensure accurate perio staging and grading over time.
Is Stage 4 periodontitis reversible?
Stage 4 periodontitis is not fully reversible because lost bone and attachment do not naturally regenerate. However, with specialized treatment, disease progression can often be controlled. Stabilizing advanced periodontal disease may involve deep cleaning, surgery, or regenerative procedures to preserve remaining teeth.
How does smoking affect periodontal grading?
Smoking is a major risk factor in periodontal classification. It typically increases the grade because it raises the likelihood of rapid disease progression and reduces healing capacity. Smokers often experience deeper pockets, more bone loss, and less predictable treatment outcomes compared to non-smokers.
Do I need surgery for Stage 3 periodontitis?
Not always. Stage 3 periodontitis may first be treated with scaling and root planing and close monitoring. If deep pockets or bone defects persist, surgical therapy may be recommended. The decision depends on pocket depth, bone loss patterns, and how well you respond to initial treatment.
How often should periodontal maintenance be scheduled?
Most patients with a history of stage and grade periodontitis benefit from periodontal maintenance every three to four months. This interval helps disrupt harmful bacteria before they cause further damage. Your exact schedule depends on your periodontal staging, grading, and individual risk factors.
Schedule a Comprehensive Periodontal Evaluation
If you’ve been told you have gum disease or are unsure about your periodontal staging and grading, a specialist evaluation provides clarity and a precise treatment plan. At Beverly Hills Periodontics & Dental Implant Center, we perform detailed exams using current AAP staging and grading guidelines to determine the exact stage and grade of periodontitis.
Your visit includes advanced diagnostics, a review of your medical history, and a personalized discussion of findings related to comprehensive periodontal disease evaluation and treatment. We serve patients throughout Beverly Hills and the greater Los Angeles area who want expert, evidence-based care from a board-certified periodontist.
Early, accurate periodontal classification can help prevent further bone loss and protect your long-term oral health. Take the next step with a trusted local specialist.







Recent Comments